AI in Diabetes Care: Past, Present & Future

Abstract
This blog delves into the future of AI in diabetes care, certifying its current implementations and tracing its historical evolution. It sheds light on the promising trajectory of AI in diabetes care, highlighting innovations such as Case-Based Reasoning (CBR), Clinical Decision Support Systems (DSS), health guidance by ChatGPT, and the integration of Machine Learning (ML) and deep learning in diabetes management.
Presently, AI has become integral to diabetes management, featuring FDA-approved devices like Continuous Glucose Monitoring (CGM) and closed-loop insulin pumps. As we embrace this evolving landscape, AI developers will continue to shape a future where technology optimally serves the complex needs of diabetes patients globally.
Transformative Role of Artificial Intelligence in Diabetes Care
In the ever-evolving diabetes care ecosystem, artificial intelligence emerges as a transformative force, offering precision, personalisation, and efficiency in treatment strategies.
The convergence of machine learning algorithms, wearable devices, and real-time data analytics has ushered in a new era in patient-centric diabetes management.
This blog embarks on an exploration anticipating the promising future of AI in Diabetes Care while tracing its footsteps through the past and unravelling its current impact.
Latest Innovations and Upcoming Prospects in AI in Diabetes Care
The future of artificial intelligence in diabetes care is poised to revolutionize the management and treatment of this chronic condition, ushering in an era of personalised and proactive healthcare.
Here are some arenas where AI in diabetes management is likely to provide a significant impact in the future.
1. Case-Based Reasoning (CBR)
Case-based reasoning in diabetes care is an experience-based approach to resolving new problems. This method builds computational memories through analogical reasoning to find solutions to similar issues.
CBR helps control blood sugar, suggesting prior-experience-based approaches to solve the latest problems, and remembering the effective and ineffective solutions for individual patients.
Roger Schank and his students at Yale University pioneered CBR implementation in the early 1980s. The four main steps of CBR include: retrieve, reuse, revise, and retain.
- Retrieve: Retrieve relevant cases from a library through keyword searches or other forms of data mining.
- Reuse: Reuse old cases to solve the current problem.
- Revise: Revise the old solution to better fit the target problem.
- Retain: Retain the newly developed solution for future use.
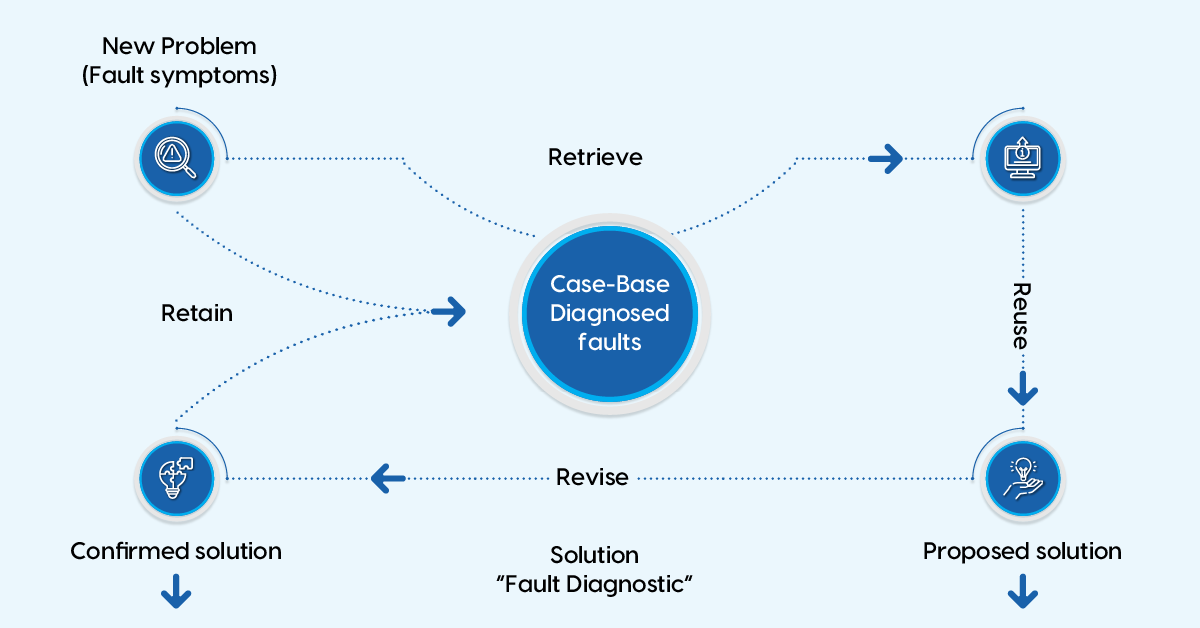
Fig 1: The 4 steps of CBR by Joaquim Meléndez
2. Machine Learning and Deep Learning in Diabetes Care
Machine learning and deep learning techniques are widely used to build digital support in diabetes care. Deep Neural Networks (DNN), Support Vector Machines (SVM), k-Nearest Neighbors (KNN), Decision Trees (DT), and Random Forests (RF) are prominent deep learning models for diabetes management.
In these models, each layer corresponds to a level of learned knowledge, ranging from low-level details to higher abstract concepts.
3. Decision Support System (DSS)
Clinical DSS implements computer programs to analyse large datasets for the timely delivery of information. This AI tool aims to improve care quality and clinical outcomes by transforming data into knowledge or meaningful advice through a digital interface.
DSS has immensely contributed to individual patient management and comprehensive screening for diabetes.
A 2018 review of 70 inpatient studies by Julian Varghese et al demonstrated positive patient outcomes via clinical DSS. Among these 70 studies, 14 were related to blood glucose management, and 70% of them demonstrated positive outcomes.
Another 2020 review of diabetes-related DSS revealed that technology interventions reduced fasting, postprandial glucose, and HbA1c levels in diabetes patients.
4. Diabetes-related health guidance via ChatGPT
ChatGPT by OpenAI can augment diabetes care by offering on-demand answers to patients’ queries based on large language models (LLMs). Currently, ChatGPT has also passed the U.S. Medical Licensing Examination reinforcing its diabetes self-management and education (DSME) portfolio.
Recently, Zhen Ying et al conducted a retrospective dataset evaluation on ChatGPT to explore its feasibility in diabetes education. The researchers asked 85 questions to ChatGPT covering seven aspects of diabetes education and ChatGPT scored high on correctness, relevance, helpfulness, and safety parameters.
Present Implementation of AI in Diabetes Management
AI and Diabetes Management witnessed a transformative revolution following the AI boom in 2021. Currently, multiple FDA-approved AI-based medical devices are implementing AI/machine learning technology. Listed below are some practical implementations of artificial intelligence in diabetes treatment.
1. Continuous Glucose Monitoring (CGM)
CGM devices monitor blood sugar at regular intervals painlessly. Currently, doctors recognize three types of CGM gadgets: intermittently viewed CGM (iCGM) and real-time CGM (rtCGM) gadgets.
While iCGm provides glycaemic information on demand retrospectively, rtCGM offers real-time data for diabetes management. Moreover, rtCGM-integrated insulin pumps enable timely insulin infusion based on real-time glycaemic values.
2. Insulin Pumps and Closed Loop Delivery Systems
Insulin pumps are a sought-after therapeutic option, especially for managing T1DM. The latest continuous subcutaneous insulin infusion (CSII) pumps come with a bolus calculator and automatic basal rate suspension to reduce hypoglycaemia.
Scientists are working towards subcutaneous closed-loop system development. STG-55 (Nikkiso, Tokyo, Japan) and its predecessor, the STG-22 are the only commercially available fully closed-loop insulin pumps in today’s market. Automated insulin delivery (AID) will improve the time in the target glucose range with either no increase or a reduction in hypoglycemia.
3. Diabetes screening via analysing ECG, Radiographs & Voice Samples
It is now possible to predict T2DM by studying electrocardiographs (ECG), frontal chest radiographs, and even voice analysis via smartphone apps.
Anoop R Kulkarni et al detected diabetes and pre-diabetes from ECGs with 97% accuracy. Ayis Pyrros et al in a 2022 study analyzed 271,065 chest radiographs (CXRs) from 160,244 patients for opportunistic screening of T2DM.
Another study involving 267 participants and 18,465 recordings stressed significant differences in voice samples of people with and without diabetes.
Scientists could predict diabetes with 75% accuracy among women and 70% among men via 5-fold cross-validation in the age-matched and BMI-matched recordings.
Similarly, it is possible to predict the onset of T2DM by metabolic fingerprinting on retinal pigment epithelium thickness.
Researchers established that a reduction in vivo measurements of retinal pigment epithelium thickness (RPET) is a crucial risk factor for T2DM. They even identified 64 RPET metabolic fingerprints that are independently associated with reduced RPET.
The advent of AI in Healthcare
The term “artificial intelligence” first came into consideration during the Dartmouth College conference proposal in 1955. However, AI applications were introduced in healthcare in the 1970s, when an AI program, MYCIN, aided blood infection treatments.
Finally, in 1979, the American Association for Artificial Intelligence came into existence, currently known as the Association for the Advancement of Artificial Intelligence (AAAI).
In conclusion, the trajectory of artificial intelligence (AI) in diabetes care is nothing short of transformative. Looking forward, the potential uses and future prospects of artificial intelligence in diabetes treatment are vast and promising.
Roger Schank’s CBR offers an experience-based approach to diabetes management, DSS harnesses the power of AI to analyze large datasets, while CGM devices and insulin pumps showcase the tangible impact of AI in real-world healthcare scenarios.
Today, AI stands at the forefront of diabetes care, promising a future marked by unprecedented advancements in treatment strategies and patient outcomes.
Key Takeaways
The abstract encapsulates the collaborative efforts shaping the landscape of AI in healthcare, emphasizing the potential for unprecedented advancements in diabetes treatment strategies and patient outcomes on the horizon.
The key takeaways include:
- The integration of artificial intelligence (AI) in diabetes care heralds a patient-centric paradigm, ensuring precision, personalization, and enhanced efficiency in treatment strategies.
- Case-Based Reasoning (CBR) emerges as an innovative approach to problem-solving in diabetes care.
- Machine learning and deep learning techniques, including Deep Neural Networks and Decision Support Systems, are transforming diabetes care by analysing large datasets.
- ChatGPT by OpenAI can augment diabetes care by offering on-demand answers to patients’ queries based on large language models (LLMs).
- AI extends its reach beyond traditional glucose monitoring, utilising diverse data sources such as ECGs, radiographs, and voice samples for diabetes screening and prediction.
About Us
Fitterfly is on a mission to fuel the global metabolic health revolution through the power of Digital Therapeutics (DTx). We partner with physicians to deliver advanced customised digital therapeutics solutions aimed at enhancing the health outcomes of their patients.
By partnering with Fitterfly, you can save time in your clinics, ensure continuity of care for your patients, get research publications, and also enhance your revenue. To know more, please fill out the form below or call us at 080-47093933.
This blog provides general information for educational and informational purposes only and shouldn't be seen as professional advice.
Want to know how can Fitterfly enhance your practice and improve patient outcomes?




















